In 1854, John Snow made quite the name for himself by halting an outbreak of Cholera in London. He famously had the city remove the handle from the Broadstreet pump, thus stopping people from becoming further infected with the water-borne illness. This summer, we had our own version of John Snow's problem...the difference was that we were dealing with a eukaryotic organism instead of a prokaryotic bacterium. Oh yeah, and people aren't dying of our disease, just getting really, really sick...and we aren't in London...and we have much more advanced ways of studying and halting the spread of infectious diseases...and okay, it's not the best analogy I suppose. The point is, we have an outbreak on our hands that has grown rapidly in the midwest and we really need to figure out which pump is housing our contaminated water...or to be more accurate, what type of produce is most likely to be the carrier for this parasite.
 |
| Cyclospora cayetanensis in various stages of development. |
Taxonomy
The scientific name of the parasite is Cyclospora cayetanensis. It is a type of unicellular organism within the phylum Apicomplexa. It belongs in class Conoidasida because it possesses a structure known as a conoid. It is further classified in the subclass Coccidiasina and the order Eucoccidiorida. These organisms are commonly called simply "coccidians". Another well-known coccidian is Toxoplasma gondii, which can cause problems in pregnant women and people with compromised immune systems. (I'll stop right there about T. gondii...otherwise we would be here all day as that is one of my all-time favorite parasites.) C. cayetanensis is placed in the family Eimeriidae with many coccidians of veterinary importance, such as Eimeria tenella, which infects chickens.
Life Cycle
 The life cycles for these protists involve direct contact with infected feces. People most often pick it up by eating foods or drinking water contaminated by infected feces. When a sick person deposits feces, the protists exist in a life stage called an oocyst. These oocysts spend a few weeks outside of a host undergoing morphological changes until they develop the necessary parts to become infective. This developmental process is called sporulation. After sporulation, a host eats whatever the parasites are contaminating and the process repeats itself.
The life cycles for these protists involve direct contact with infected feces. People most often pick it up by eating foods or drinking water contaminated by infected feces. When a sick person deposits feces, the protists exist in a life stage called an oocyst. These oocysts spend a few weeks outside of a host undergoing morphological changes until they develop the necessary parts to become infective. This developmental process is called sporulation. After sporulation, a host eats whatever the parasites are contaminating and the process repeats itself.Cyclosporiasis
The disease caused by C. cayetanensis is often called "traveler's diarrhea", but the medical term is cyclosporiasis. Symptoms typically include fatigue, nausea, flatulence, and anorexia followed by watery stools, abdominal cramping, low-grade fever, gastroenteritis, and weight loss. If left untreated, these symptoms can persist for about 57 days.
Diagnosis
The diagnosis of cyclosporiasis is fairly difficult because these protists are small and difficult to stain. There are four commonly accepted methods for diagnosing this disease:

1-Finding it in a fecal smear (a.k.a. checking the poop)
2-Finding that these parasites are undergoing sporulation
3-Finding parasites in bowel biopsy or intestinal fluid.
4-Good old PCR (polymerase chain reaction).
The parasite also auto-fluoresces (glows) under a black light. So using a UV light while performing microscopy can also be helpful for diagnosis.
Treatment
Despite the nasty symptoms, this infection is fairly readily cured. Current protocol describes using antibiotics (like trimethoprim-sulfamethoxazole for instance). These drugs are administered over the course of about 7 days. If left unchecked for too long, or if the infection is very severe, some people do have to be hospitalized. Luckily, very few people ever die from this disease.
Prevention
The best way to prevent contracting this parasite is to always thoroughly wash any produce that you have (especially raspberries, as you will see in a moment) and to make sure that you are getting clean water when traveling to countries with sanitation problems. These parasites are often contracted by people traveling in Peru, Brazil, and Haiti, but if you know your water is coming from a reliable source and your produce is properly washed, you should be fine. Outbreaks have occurred in the U.S. and in Canada from fruits imported out of Central and South America.
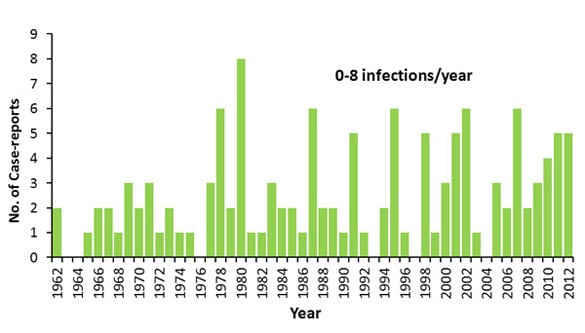
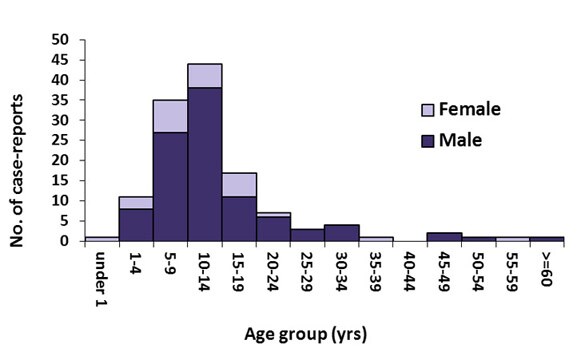
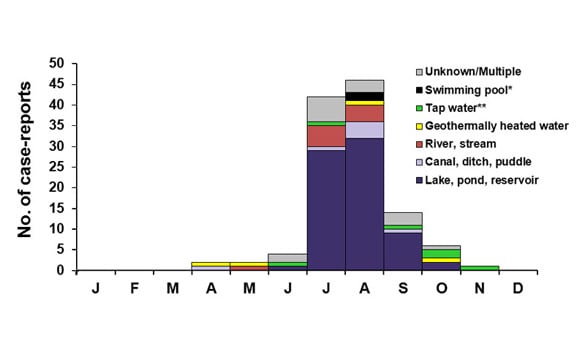
Recent Outbreaks
The most recent outbreak began in Iowa during June of this year. When I first read about the outbreak, there had been 22 cases reported. As of today, there have been 138 confirmed cases in Iowa. Many other states have seen an increase in cases as well. Nebraska jumped from 16 cases a few weeks ago (11 cases coming out of Douglas Co.) to 70 cases as of this morning. My home state of Texas has seen 66 cases. Georgia has reported 2 while Wisconsin has reported 3, and single infected individuals have popped up in Kansas, Ohio, Illinois, Minnisota, New Jersey, and Connecticut. That brings us up to 285 cases spanning 11 states in the last month. Ten of these people wound up in the hospital and who knows how many cases have gone unreported. This is certainly well above the average number of annual cases which has been around 150 for the last eight years according to the CDC. So far, no one has been able to determine what is causing the outbreak, but the best guess is some type of imported fruit was tainted.
 |
| Risk Areas for Traveler's Diarrhea: Green=Low, Off-White=Intermediate, Red=High |
Less Recent Outbreaks
 |
| Someone had fun with Photoshop. I thought this was pretty clever. |
Moral of the Story
The biggest lesson learned from doing research for this post is that you should ALWAYS thoroughly wash your produce. These little guys can't burrow their way into the foods they are contaminating, so giving your fruits and veggies a good wash is really all it takes to save you from 57 days of things coming out of both ends. Also, if you are traveling, take extra care in paying attention to where your food and water are coming from. Finally, if you live in any of the areas in or around outbreak zones, be sure to see a doctor if you start to experience any of the symptoms of this disease. Get yourself a strong dose of antibiotics and be glad you only had to suffer 7 miserable days of illness instead of 57! Where is John Snow when you need him? I bet he'd know nothing about cyclosporiasis anyway...(that may or may not have been a Game of Thrones reference...).
 |
| Is his name Guatemala? No? Alright, we'll blame Lone Star! |